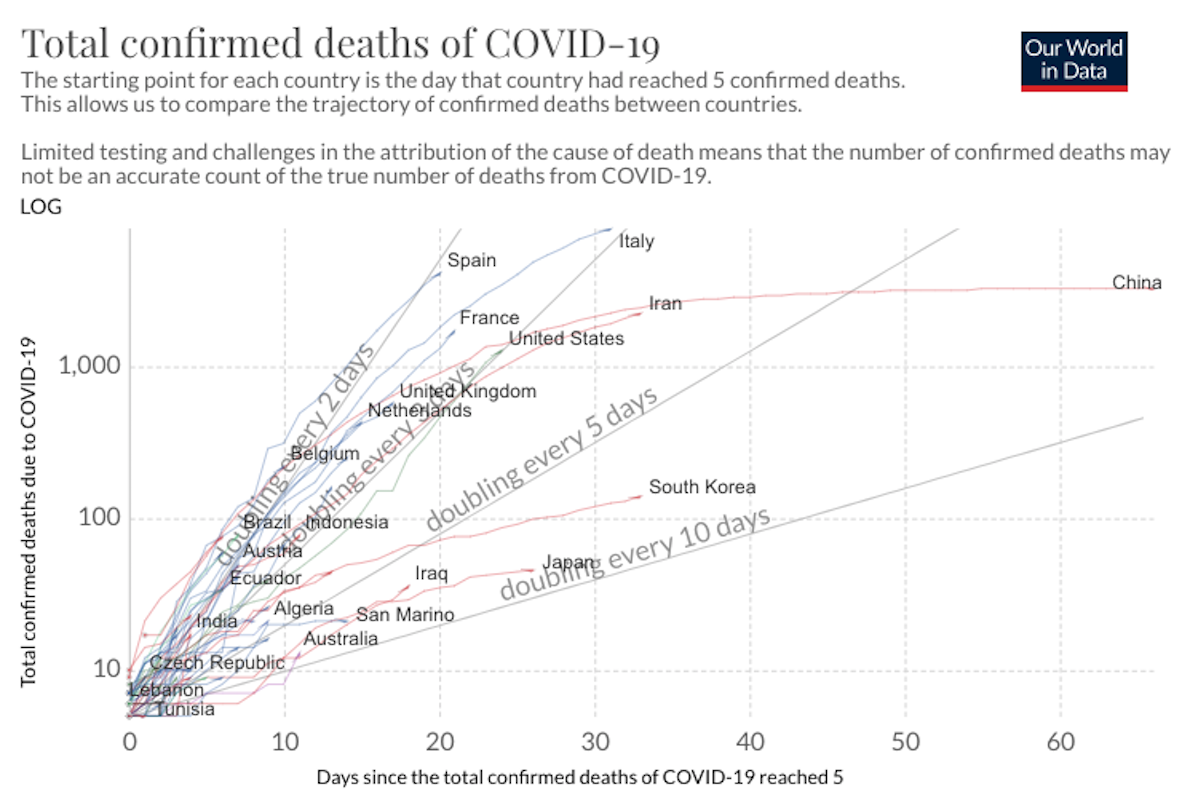
COVID-19 Science Update for March 27th: Super-Spreaders and the Need for New Prediction Models
Absent isolation or other precautionary measures, the average socially active COVID-19 infectee will transmit the disease to an average of about 2.4 people. i.e., the R0 value is 2.4. But super-spreaders can spread a disease to dozens or hundreds.
· 11 min read
Keep reading
Manosfear
Robert King
· 17 min read
Anti-Zionism as Redemptive Racism
Shalom Lappin
· 15 min read
Treacherous Men
Ronald Radosh
· 12 min read
Never Neverland
Andrew Hammel
· 32 min read
Homeric Heresies
Cathy Young
· 11 min read