Activism
First, Do No Harm: A New Model for Treating Trans-Identified Children
Individuals with a fragile ego structure also tend to be prone toward black-and-white thinking, which leads them to concrete rather than symbolic solutions.
We are two psychotherapists, husband and wife, with professional involvement in the therapeutic treatment of trans-identified individuals in the UK. The material that follows is connected to a paper we presented at a multi-disciplinary conference on January 23rd, Do Not Adjust Your Set: Sex, Gender And Public Policy, and reflects our serious concern about the transition of children before maturity—though, as we would like to emphasize, we are not taking a position in regard to an adult’s right to transition. Indeed, we understand that transition is, for some adults, the optimum way to lead their lives and present to the world. In all cases, we encourage a psychotherapeutic model that provides a process of psychological exploration, in which an individual’s personality structure, beliefs, defence mechanisms, and motivations are assessed and examined in a supportive environment. All of these elements, we believe, are helpful for anyone planning this kind of life-altering decision.
Between 2003 and 2007, I, Susan Evans, worked for the Gender Identity Development Service (GIDS) at the Tavistock Clinic in London, a specialised facility for young people experiencing difficulties with gender identity. During this period, I became concerned that some of the children were being referred for hormone treatments after a fairly superficial assessment process. Asking questions or holding a discussion about this felt uncomfortable. Although we were running a clinical service, there sometimes was little meaningful exploration of the presentation of our patients. Eventually, I decided to speak to the medical director of the Tavistock and Portman NHS Foundation Trust, under whose auspices GIDS operates. Shortly thereafter, an internal inquiry, conducted in 2005 and 2006, recommended that the service should carry out more rigorous investigation and research in regard to gender dysphoric children. Yet nothing substantially changed. Eventually, I resigned from the clinic, though I continued to work elsewhere within the Tavistock Trust.
In 2018, my husband (and co-author) Marcus was elected as a Tavistock Trust board governor. In this capacity, he became aware of two issues that touched on my own concerns. The first was described in a letter from a group of concerned parents regarding the quality of the treatment their children had received at the gender clinic. The second was a report authored by Dr. David Bell, who, in his role as staff governor, had been approached by a group of 10 GIDS professionals (about 20 percent of the total staff) expressing ethical concerns consistent with the issues raised by the parents. Marcus resigned in February 2019 because he didn’t believe the Trust’s leadership intended to take these concerns seriously. It was around this time that politicians and journalists began exploring this policy area more vigorously, too—including at a May 2019 House of Lords event titled “First Do No Harm: The ethics of transgender healthcare.” I attended that event, and found the presentations deeply concerning.
After the event, several of the participants met informally, whereupon we discussed how to get past the apparent lack of interest from the National Health Service in ensuring that clinical safeguarding and ethical practices were respected. One problem, we all agreed, was that there was a serious reluctance among many professionals to speak out publicly, lest they be accused of transphobia. Journalists covering the issue had reported that they had trouble finding anyone to go on the record. This situation persisted for months, even after the BBC’s Newsnight division published investigative reports that demonstrated all was not well at GIDS.
Marcus and I were being contacted by parents and ex-patients, many with tales of upsetting (and sometimes harrowing) treatment experiences. They expressed thanks that at least a few professionals were speaking out about a treatment model that they felt was doing harm. One of the parents was Mrs. A (as identified in the judicial review), a mother who had a 15-year-old daughter who’d been diagnosed with autism, and was experiencing emotional difficulties. The daughter also had decided she was transgender, and was on the waiting list for GIDS. Mr. and Mrs. A were worried that their daughter would be started up on hormone treatments without first receiving a thorough psychological assessment and treatment.
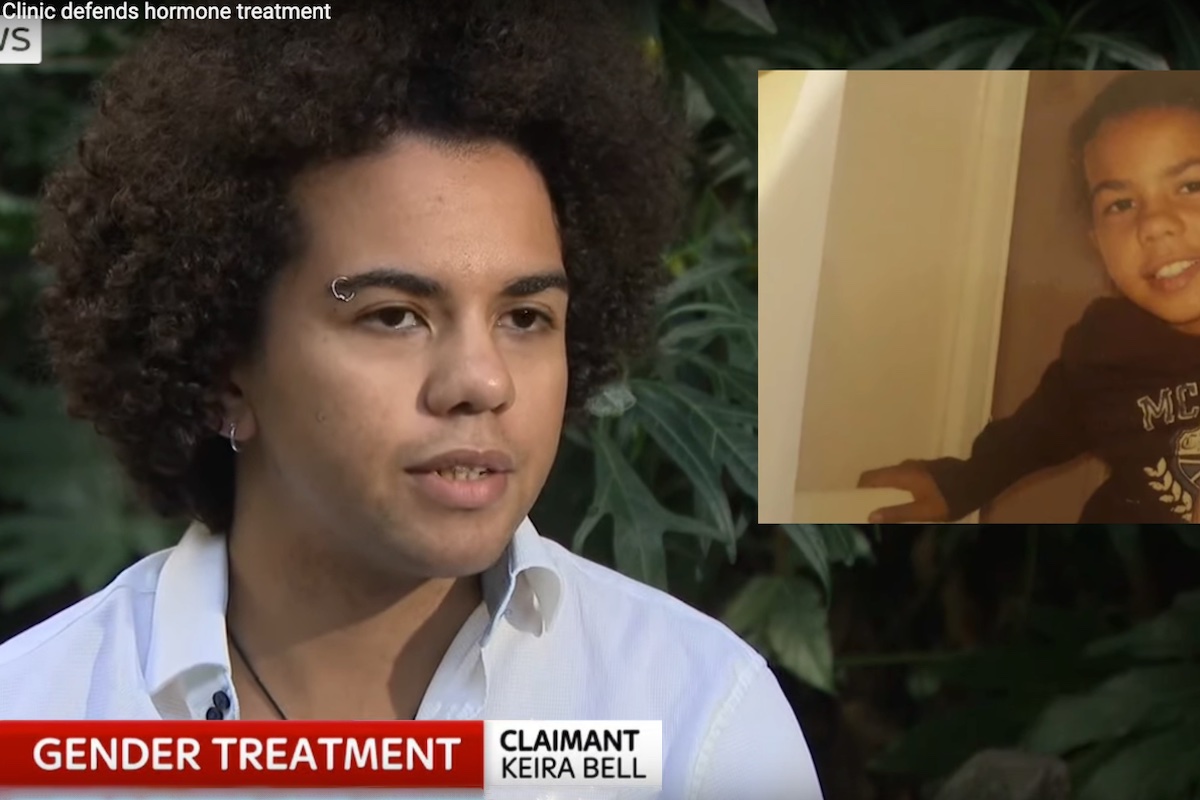
By now, we knew that raising concerns through formal channels at the Tavistock would likely be fruitless, as its leadership seemed incapable of any kind of institutional self-examination that conflicted with the established dogma of (1) speedily “affirming” a trans-identified child’s announced identity, and (2) claiming, without evidence, that puberty blockers are “fully reversible.” So, following a consultation with a legal team, Mrs. A and I agreed we would request a judicial review as to whether children can indeed give informed consent to hormone blockers. In October 2019, we applied to the High Court, and the request was accepted. We then started gathering a multinational group of expert witnesses, one of whom was Keira Bell, a name many readers will know. Keira—now a 23-year-old detransitioner (i.e., someone who once presented as transgender, but no longer does so) believed that her co-morbid psychological difficulties had not been sufficiently assessed or treated at GIDS before she was started on blockers and cross-sex hormone treatments at the age of 15.
In January 2020 our evidence was submitted at the Royal Courts of Justice in London for review. Then in February, Keira took my place in the case, joining with Mrs. A as co-claimant. In October, the three-judge review took place at the High Court. And on December 2nd, the judges ruled against the Tavistock GIDS, and put limits on GIDS’s ability to medically transition non-adults. In their judgment, they concluded that it was “highly unlikely” a child under 13 could give informed consent to such treatment; and that, even in regard to those aged 14 or 15, “doubtful” that they fully understand the implications of these medication regimes. The judges added that it would be appropriate for clinicians to involve the court in any case where there may be doubt as to whether the long-term best interests of a 16- or 17-year-old would be served by such clinical interventions.”
But of course, our goal was never to make it more difficult for gender dysphoric children and their families to obtain help and treatment. What we wanted was for these families to get the right treatment. There is currently no gold standard, long-term research in the area of childhood medical transition. Carl Heneghan, Director of the University of Oxford’s Centre for Evidence-Based Medicine and Editor-in-Chief of BMJ Evidence-Based Medicine, has called puberty-blocking treatments “an unregulated live experiment on children.” And so, in parallel with the above-described legal process, Marcus and I set about creating something substantial to help children, parents, and professionals faced with these cases. This took the form of a book manuscript, due to be published this spring. This article offers a précis of the ideas that the book will contain.
* * *
A wish to transition is often described by those who experience it as a belief that they were “born in the wrong body,” and consequently deprived of an idealized relationship with their physical self. The ideal we all have, at some level, is a self that would be loved and accepted by others, and by ourselves. In this ideal state, it is hoped, an individual would be free of the usual sorts of mental pain, conflicts, and humiliations. It’s understandable that parents and professionals want to protect children from unnecessary pain and give them something that the child believes will make them feel more comfortable. However, it’s important that parents and professionals help the child assess the level of pain or discomfort they experience. The child needs to develop a capacity to notice pain, because it can represent a helpful indication of something that needs attention. But they also need help differentiating the type, degree, and cause of pain. The desire to reduce pain and anxiety by rushing into either social or medical transition needs to be resisted, as there are long-term costs that a child in a fixed state of mind is unable to imagine or understand.
It’s worth re-emphasising the importance of not separating gender dysphoria from other aspects of a person’s mental functioning, since many of the young people who present with gender incongruence have co-morbid problems. The denial of the psychological factors influencing the desire to transition can unwittingly lead the patient and health professionals to embrace concrete, affirmative solutions, while ignoring relevant aspects of the individual’s mental-health situation and personal history.
Many children who are drawn to the idea of transition have a fragile ego structure that threatens to fragment if overwhelmed by psychic pain. And like other individuals, they can experience daydreams in the vein of “If only I were…” to help manage the emotional struggles of day-to-day life. A trans-identifying child can become more fixated and invested in the daydream idea, and it becomes a belief that if only they’d transition, all their problems would resolve.
Individuals with a fragile ego structure also tend to be prone toward black-and-white thinking, which leads them to concrete rather than symbolic solutions. This also makes them susceptible to the somewhat rigid thinking and stereotypes that now characterize the more stridently promoted elements of trans-rights activism and its associated ideological components.
We also have found that the desire to transition often is related to a wish to control sexual development, and perhaps to defer it entirely—including in a literal sense, through the use of puberty blockers. It’s interesting to note that many detransitoners report that there is little talk about sex on pro-transition websites, or in the medical care they received. Under the current “affirmative” model of treatment (which might more aptly be called a “belief-confirmation” model), some services may be tacitly providing reassurance to young people that their anxieties about sexual development will be removed through gender transition. We would argue, however, that adolescent confusion and distress is a normal and even necessary part of development. And over time, the adolescent can be helped and supported to become an adult who might enjoy what their natal sexual body has to offer.
When a person states they are trans, or reports gender dysphoria, it is important for a therapist to listen to the individual and explore what is occurring within their life. The presentation and message from the patient can, at first, be fixed and one-dimensional. Rather than the patient presenting a distressing psychological symptom, they more usually talk of feelings of detachment from, or discomfort with, the body they were born in. This includes stating that their bodies contain unwanted aspects of the self—represented, for example, in boys by their Adam’s apple and hairy legs, and in girls by breasts and the onset of menstruation.
But although medical interventions may interfere with the body and block its sexual development or functioning, such interventions cannot completely eradicate a patient’s natal gender. This might lead to a sense of persecution, as the body is a constant reminder of the continued existence of the unwanted aspects of the self. This persecution often is projected onto others whose position of neutrality—or even curiosity—is experienced as an externalized expression of their own internal doubt about the authenticity of their transition. This sense of persecution also manifests in extreme reactions to misgendering, “deadnaming,” or other external reminders of one’s natal body.
Patients often put enormous pressure on family, schools, and clinical services to adhere to their own belief that transitioning to an idealized body will solve their problems, and that failure to comply will cause them trauma. Family members and clinical services are pressured to support the patient’s belief that his or her psychic problems can be dealt with by interfering with the body’s appearance and functioning. And many do come to believe that the most humane course of action is to help alleviate the individual’s distressing symptoms of gender dysphoria with affirmative therapy. But there is evidence that this can further cement the trans identity—rather than allow for some acceptance of one’s natural body and gender (which would allow the individual to avoid the medical risks of hormone therapy). As in many other areas of health care, long-term problems arise when clinical staff feel forced to provide a quick solution.
All human beings are complicated. And our problems are usually multidimensional. This is why therapists need to take an interest in the meaning of a patient’s presentation, as well as explore the dynamics underlying the presenting belief system. Unfortunately, for reasons described above, any exploratory stance whatsoever can be experienced as disturbing or even offensive to gender-dysphoric patients. This is because it threatens to undermine their internal defences and belief systems. The therapist therefore needs to demonstrate respect and empathy in understanding the role that these defensive structures play in supporting the patient’s ego and managing his or her anxiety.
Two of the current diagnostic criteria for gender dysphoria are the demonstration of persistence (over time) and consistence (in self-conception) in one’s gender identity. But we question the value of these diagnostic categories when forming a care plan for a young person. The accuracy of mental-health diagnosis in children is notoriously unreliable prognostically, as children change during the course of their development. Children who are diagnosed with one thing at a particular age may turn out very differently when they reach maturity. Many young people with gender dysphoria appear to be frozen in their current preoccupations. And by the time they present for transition, they typically have suppressed any of the doubts and anxieties they would naturally entertain, having instead projected them onto those around them.
We have often heard it argued by gender-services staff that a child’s certainty in his or her trans identity is a positive sign, which helps confirm that transition is the correct medical intervention. But we would actually view unblinking certainty as something of a red flag, since it isn’t expected that an individual would dismiss or ignore the very real anxieties, pain, stress, risk, and compromised body function that inevitably attend even a successful medical transition.
If a child’s “certainty” is left unquestioned by the adults around them, then it is statistically more likely that they will continue in their trans identification. But as yet, there is no proven method to determine who is “truly” trans. Many have been certain they were, and later admitted they were mistaken. Moreover, in our experience, we have found that children wishing to transition subconsciously often hope that a parental figure will step in and help to identify and understand the part of the self that they are trying to discard. Some detranstionors mention, after the fact, that they were disappointed by doctors’ and therapists’ inability to stand up to their insistent demands for transition action.
* * *
Children and adolescents have all sorts of fantasies and anxieties about the mechanics of sex and sexual roles. These desires and conflicts touch on infantile fears of being invaded or invading, being overpowered or being powerful. Because these ideas can be unsettling, transitioning can soothe a person by blocking anticipated sexual development. When working with gender-questioning patients, talk about sex and sexual fantasy has to be carefully managed and age-appropriate, of course. But notwithstanding the claim that gender and sexual impulses are entirely unrelated, it is essential to explore each person’s attitude toward sex, including the question of sexual orientation and relationships.
Discovering and understanding the real factors causing distress may help avoid the need for medical treatments. Ultimately, a psychologically healthy person needs to come to terms with his or her sexual self, and so it helps if a therapist can support the person as they begin to think about their fears and anxieties, rather than encourage them to seek avoidance mechanisms. The task of adolescence is to prepare for adulthood, not to artificially postpone it.
When a patient indicates that they wish to change names or schools to correspond with their transgender status, the therapist may feel discouraged from even mentioning the patient’s actual natal sex and identity. But that does a disservice to the patient. If a child wants to change their name from Joanne to John, the therapist should keep in mind who Joanne is and why she is so unwanted or unacceptable.
The therapist has to bear in mind that it is common for people to, at least subconsciously, seek to eradicate unwanted aspects of the self. But it is not really possible to do this, as discarded parts of the self tend to re-emerge, particularly when the ego is under pressure. Mental health is based on an ability to integrate various aspects of the self, not pretend them away, while differentiating between psychotic and non-psychotic forms of thought. This means being able to recognize the difference between reality-based thought and wishful thinking, and helping patients learn to do likewise.
Discussions with detransitioners are important, because these individuals often have attained self-awareness about these phenomena. Many report that at some level of their mind, they knew they had doubts that might contradict their stated beliefs and ideas about transition—and so they engaged in a mental form of double bookkeeping. During the period when they outwardly signalled defiant certainty about their trans identity, they actually needed an adult to help them deal with the aspects of themselves they were keeping hidden, and to allow that part to emerge.
This is not a simple on-and-off proposition: In our clinical experience, a child often can go through long phases of maintaining a fixed belief that they need to transition, while occasionally opening up and exploring their feelings in therapy, though this is usually followed by a retreat into a fixed state of mind. At these times, the therapist must try to respect the defences and wait for the patient to re-emerge. Grievances in relation to parental figures will become transferred onto the therapist relationship, and the therapist might be required to tolerate quite a bit of provocation, as their work with the individual is continually attacked and undermined by that part of the patient’s mind that’s determined to keep up a defensive front. It is helpful if the therapist can see the hatred or anger involved in these attacks as part of a developmental step—evidence of the young person’s wish to keep their psychic posture intact.
Most of us harbour grievances toward our parents for failing to provide us with an idealized mind, body, and/or environment. These grievances often are based on the belief that we would have been in a better position to deal with life if only our parents had not, for example, favoured our younger sibling or given us large ears. Changing the name chosen by a parent can represent an unconscious complaint against them: It is believed that the parents not only gave their child the “wrong body” but also gave them the wrong name. This can represent a wish to kill off the individual created by the parents, creating instead someone who has chosen their own name and their own gender. The hostility involved in grievances often is consciously denied while being communicated at an unconscious level.