Vaccines
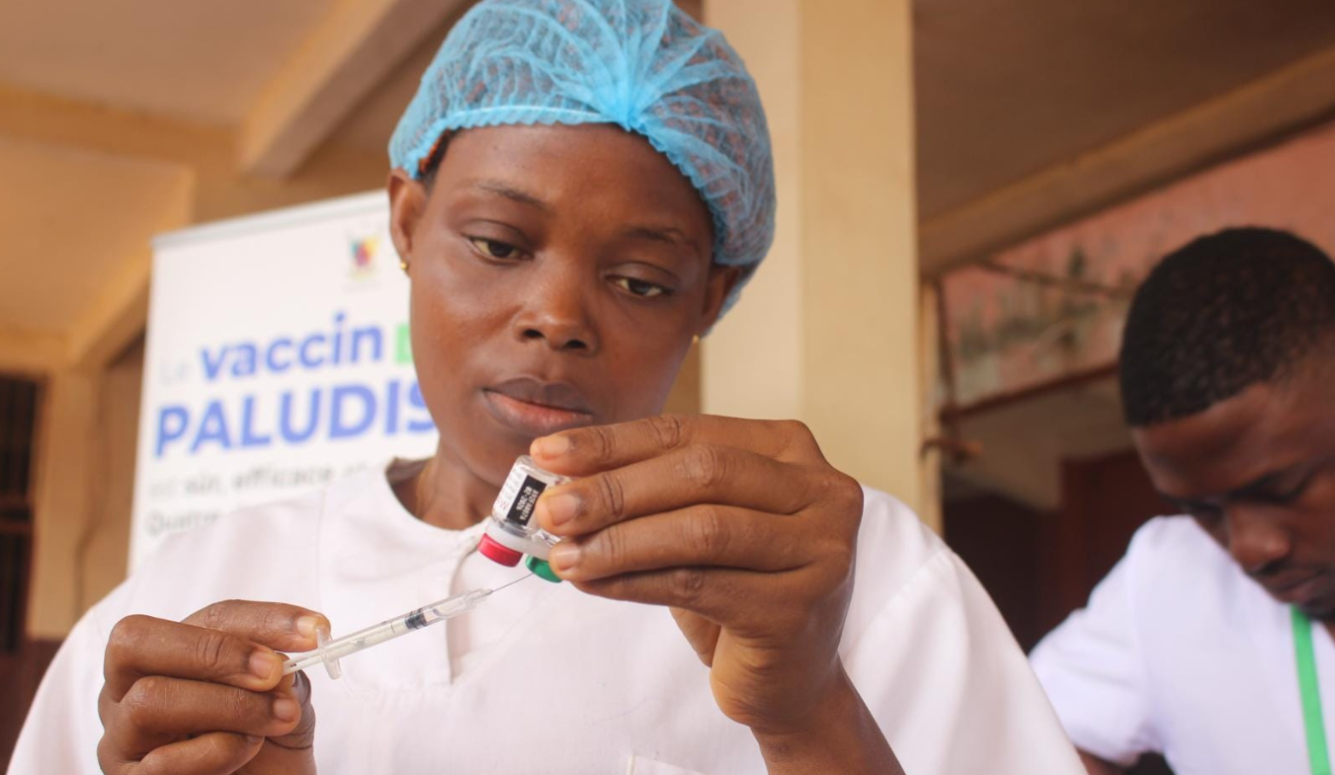
Will the New Vaccine Help Eradicate Malaria?
The malaria vaccine may well help reduce deaths, but we should not exaggerate its efficacy.
· 7 min read
Keep reading
Richard Dawkins and the Claude Delusion
Sean Welsh
· 10 min read
Open Hiding
Izabella Tabarovsky
· 7 min read
Lists, Damn Lists, and Critical Correctness
Dave Thompson
· 12 min read
Claire's Weekly Letter: Secrets and Lies
Claire Lehmann
· 3 min read
Why Epstein, But Not Jackson?
Claire Lehmann
· 5 min read




