COVID-19
COVID-19 Science Update for March 22nd: Grim Omens in the U.S.
The problem isn’t just the number of ventilators and ICU beds, but also the limited number of staff who can operate such equipment.
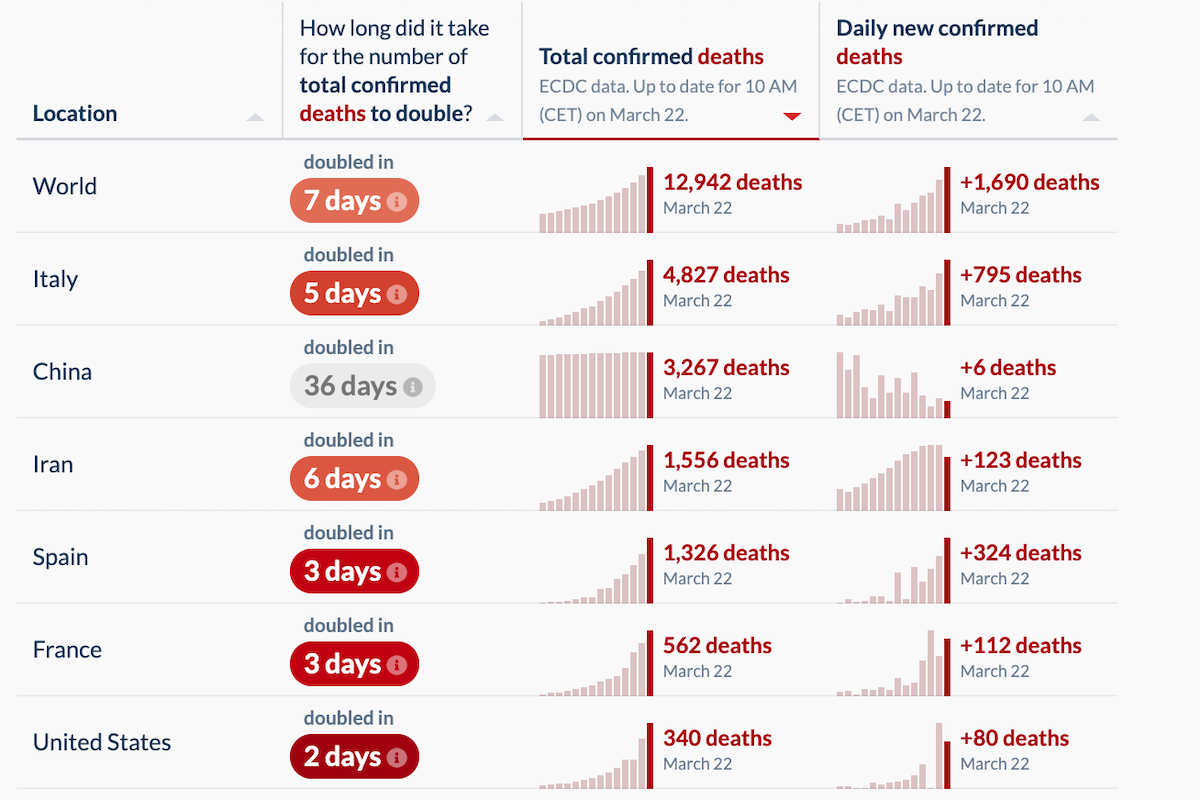
The latest global data for COVID-19—updated with reports received on March 22nd, 2020—have been published at Our World in Data. Here are some of the numbers and trends that I believe deserve special attention, as well as a brief report on notable regional developments and media analyses. Since March 21, these updates have been published at Quillette in our section marked COVID-19 UPDATES. Please report needed corrections or suggestions to [email protected].
Yesterday’s global tally of total confirmed cases was 305,275. This represents a daily jump of 34,047, up from the previous daily jump of 28,891. This includes:
- Another 6.5K cases in Italy (a slight increase from the previous daily jump);
- A worrying 4.9K case jump in Spain (up from the previous daily jump, which was 2.8K);
- And a big 7.1K increase in the United States, the biggest U.S. jump to date.
These three countries account for more than half of all new cases. If you add in France (1.8K) and Germany (3.3K), you get more than two thirds of global cases.